Ear infections can occur in the outer or middle ear. An ear infection occurs in the middle ear when fluid becomes trapped following a viral or bacterial infection. This painful affliction is most common in children, but can affect people of all ages. Infections can also occur in the outer ear. They are most common when the skin in the outer ear is dry and cracked. Ear infections can be either acute (of short duration) or chronic (persisting or reoccurring frequently).
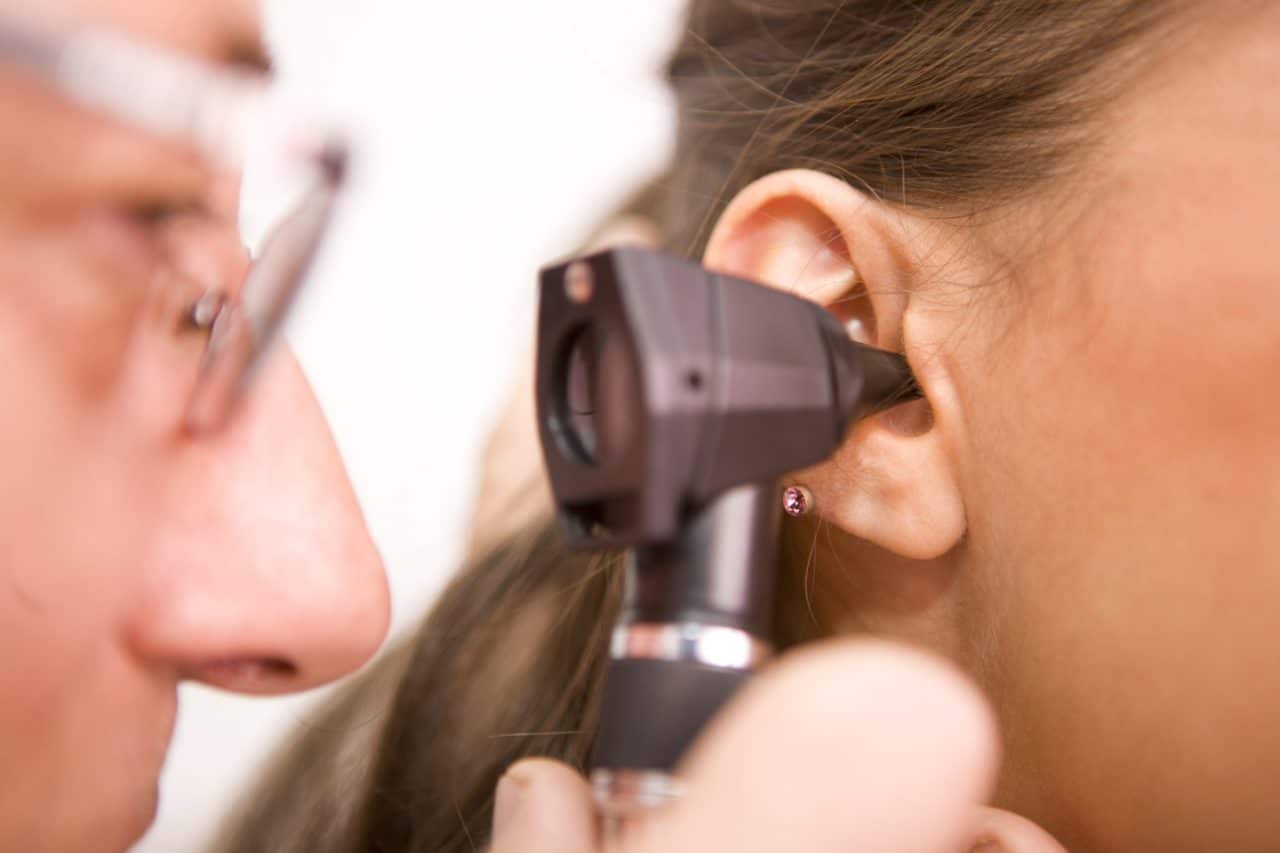
What Causes Ear Infections?
Otitis media is the medical term for an inflammation of the middle ear, commonly referred to as an ear infection.
The majority of ear infections are viral or bacterial in nature, usually occurring after a cold or upper respiratory infection. These conditions cause swelling of the Eustachian tube, a small canal that connects the middle ear to the nostrils and provides an outlet for fluid drainage, trapping germs and fluid in the middle ear and leading to infection.
Because children are still growing physically, some of their internal organs may also be temporarily underdeveloped. This is true of the Eustachian tube, the vertical canal that connects the middle ear to the nostrils, providing an outlet for fluid drainage. Eustachian tubes in children are still horizontal and therefore don’t drain the fluid efficiently.
Because the Eustachian tube is smaller in children, it is more prone to swelling; when this occurs, fluid is trapped in the middle ear. This fluid presses against the eardrum, causing pain, and can harbor germs that lead to infection. The result is an earache and, in some cases, loss of hearing. When the infection does not completely go away or returns often, it is referred to as chronic.
What Are the Symptoms of an Ear Infection?
The hallmark signs of otitis media are pain and pressure in the ear and fluid drainage. These may be accompanied by a low-grade fever and hearing loss. Infants are often fussier than usual, and may cry inconsolably, refuse to eat and have trouble sleeping. They may also pull or tug on the ear. Symptoms may be milder in chronic ear infections. Should your child display any of these symptoms, bring them to the doctor; the sooner an acute ear infection is treated, the lower the chances of it developing into a chronic condition.
How Are Ear Infections Treated?
Treating an ear infection begins at home. To help soothe symptoms, gently press a warm washcloth against the affected ear. You may give your child eardrops and over-the-counter medications such as acetaminophen or ibuprofen to help relieve pain. Avoid aspirin, which can be dangerous to young children.
Your child’s doctor will likely prescribe antibiotics to treat a chronic ear infection. These should be taken until used up, even if your child’s symptoms appear to be improving; otherwise, the infection could worsen.
When medication is not effective, a surgical solution involving ear tubes may be considered. These are inserted in the middle ear and provide ventilation and fluids, keeping the ear clear and preventing infection. Most ear tubes remain in place anywhere from six to 18 months and eventually fall out on their own. If not, surgery to remove them is performed.
Can Ear Infections Cause Complications?
If left untreated, chronic ear infections can lead to a variety of complications including hearing loss, damage to the bones in the middle ear, balance problems, a middle ear cyst called a cholesteatoma, facial paralysis and inflammation of the brain. For these reasons, early detection and treatment are crucial. Better still is prevention.
You can’t always stave off an ear infection, but there are steps you can take to reduce the chances of your child developing one. These include breast-feeding your baby, making sure they are up-to-date on vaccinations, practicing good hygiene (e.g., regular hand-washing), keeping your child away from tobacco smoke, and enrolling them in as small a day care or preschool facility as possible. Simply put, fewer children mean fewer germs.
Otitis media is the medical term for an inflammation of the middle ear, commonly referred to as an ear infection. It is the result of fluid becoming trapped behind the eardrum, and is usually caused by a virus or bacteria. People of all ages can develop ear infections, but they are far more common in children than older adults: three out of four children will experience at least one ear infection by the time they are three years old.
Otitis media is characterized as being either acute or chronic. Acute cases are most common; they come on suddenly but last for only a short duration. Chronic otitis media occurs when fluid remains in the middle ear or returns repeatedly.
What Causes Otitis Media?
Bacteria and viruses are the leading causes of ear infection, which often follows on the heels of a cold, sore throat, or upper respiratory infection. Colds, flu, and strep throat frequently lead to otitis media. Germs can spread to the middle ear and become trapped when the Eustachian tube, which is responsible for draining fluid, becomes swollen or blocked due to a cold or other illness.
Children have smaller Eustachian tubes than adults, and their immune systems are still developing, making it more difficult for them to fight off infections. For these reasons, they are more likely to suffer from ear infections.
What Are the Symptoms of Otitis Media?
In addition to a painful earache, those suffering from otitis media may experience a discharge from the ear, fever, difficulty hearing, irritability, loss of appetite, trouble sleeping, vomiting, and diarrhea.
How Is Otitis Media Treated?
Treating otitis media often involves antibiotics such as amoxicillin, coupled with over-the-counter pain relievers and eardrops. Children should never be given aspirin, as it can lead to a potentially fatal disease called Reye’s syndrome. Pressing a warm compress against the affected ear can bring relief, as well.
Most ear infections run their course in a matter of days. If your child suffers from chronic otitis media that doesn’t respond to medication, surgically implanted ear tubes may be recommended.
These provide ventilation and prevent fluid from accumulating in the middle ear. They remain in place anywhere from six months to two years, usually falling out on their own. If ear tubes don’t do the trick, surgery to remove the tonsils and/or adenoids may be considered.
What Causes Earaches?
Ear pain, commonly referred to as an earache, is a common complaint and can result from infection or poor Eustachian tube function. Other causes include ear trauma, perforated eardrum, sinus infection, sudden changes in pressure, excess buildup of earwax, sore throat, shampoo or water in the ear, tooth infection, arthritis of the jaw, and a foreign object in the ear.
What Are the Symptoms of an Earache?
Ear pain is a pain in one or both ears that may be dull, sharp, or burning. It can be constant or intermittent, and is most common in children. Symptoms will vary depending up on the cause of the ear pain; however, symptoms may include redness, swelling, fever, fullness or pressure, itching, drainage, decreased hearing, tinnitus (ringing in one or both ears) and drainage.
If you are experiencing severe ear pain, dizziness, headache, a discharge of blood or pus from the ear, swelling, and facial muscle weakness, seek medical attention. If pain does not dissipate in 24 to 48 hours or worsens, or your symptoms continue, see a doctor. A sudden decrease in severe pain also warrants medical attention, as it may indicate a ruptured eardrum.
How Are Earaches Treated?
Since there are many causes of earaches, treatment will depend on the cause. Treating the cause should relieve ear pain in most situations.
In the meantime, there are steps you can take to treat ear pain at home. Apply a cold, wet washcloth to the ear for at least twenty minutes. Lay on the side with the ear that doesn’t hurt closest to the ground. Sit in an upright position to reduce ear pressure, chew on something to help relieve pain, and use over-the-counter pain relievers. Eardrops can also be administered, unless you suspect an eardrum perforation.
To help prevent earaches, refrain from inserting objects in your ears. Dry your ears thoroughly after bathing or swimming, avoid tobacco smoke, and reduce your exposure to allergy triggers such as pollen and dust.
Call Willamette ENT & Facial Plastic Surgery at (503) 581-1567 for more information or to schedule an appointment.
“Have always found the staff and doctors here to be helpful. This was my first visit with Dr. Prze after Dr. Allan retired, and he was very friendly, enthusiastic, and thorough. It was obvious he had read my chart carefully before my checkup.”